What is a CGM? Is it right for you?
What is a CGM sensor?
Why is a CGM better than other methods of monitoring blood sugar?
Is a CGM right for you?
How to use a CGM to monitor blood sugar
Downsides of CGMs
Why is it important to monitor blood sugar?
Next steps: a 4-week plan
What is a CGM? Is it right for you?

A Continuous Glucose Monitor (CGM) device, is a medical device that provides real-time monitoring of glucose levels in individuals. It is mainly used for people with diabetes. Unlike traditional blood glucose meters, which require fingerstick blood samples, a CGM continuously tracks glucose levels through a small sensor inserted under the skin, typically on the abdomen or arm. The sensor measures glucose in the interstitial fluid, which is the fluid surrounding the cells, and sends this data to a receiver, wearable or smartphone app. This allows people with diabetes to get real-time insights into their glucose levels, helping them manage their condition more effectively.
CGMs offer several advantages over traditional glucose monitoring methods. They provide continuous data, alerting the wearer if their glucose levels are too high or too low, which can help prevent dangerous situations like hypoglycemia or hyperglycemia. Additionally, CGMs can help track glucose trends throughout the day, allowing for more precise adjustments to insulin doses, diet, and exercise. Over time, this can lead to improved blood glucose control and a reduction in the risk of long-term complications associated with diabetes, such as nerve damage, kidney issues, and vision problems.
If you have diabetes, it can be vital to monitor and control your blood glucose. However, even if you don’t have diabetes, keeping track of your blood glucose levels may still be a smart idea for many people, especially obese. Increasing blood sugar and declining metabolic health are associated with a higher risk of multiple diseases, including cancer, heart disease, dementia, and even early death.
CGMs are becoming increasingly relevant in the management of obesity, particularly for individuals who may be at risk for developing type 2 diabetes, since they can offer valuable insights into how the body responds to food, exercise, and other lifestyle factors in people with obesity. By continuously tracking glucose levels, CGMs can help identify blood sugar spikes or drops that might occur after eating certain foods, thus providing critical data to understand how dietary habits influence metabolism and weight management.
For individuals with obesity, CGMs can be a powerful tool in personalizing nutrition plans. The real-time feedback helps people pinpoint which foods cause significant glucose fluctuations, enabling them to make better food choices and adopt a more balanced diet. By managing glucose levels more effectively, individuals can reduce the risk of developing insulin resistance, a key factor in obesity and the onset of diabetes. Moreover, using a CGM allows for monitoring the effects of exercise on glucose levels, helping individuals optimize their physical activity routines for better weight management.
Additionally, CGMs can provide motivation and accountability, offering tangible data that shows the direct impact of lifestyle changes on glucose regulation. This continuous feedback loop can support behavior changes over time, leading to healthier habits and potentially aiding in weight loss. Ultimately, CGMs provide individuals with obesity a clearer understanding of their metabolic health, which can be instrumental in achieving sustainable weight loss and improving overall well-being.
What is a CGM sensor?

A CGM is a small medical device that monitors your blood sugar in real-time. Most devices are incorporated in a patch that, most of the time, goes on your abdomen or upper triceps. The patch stays in place for 7 to 14 days and works by using a small sensor which reaches the interstitial fluid, the fluid that surrounds cells right under your skin. You don’t feel this thin microfilament and the risk of bleeding or infection is almost zero. The sensor sends the readings to an app on your phone or watch.
Here is how it works in more detail:
Sensor Insertion: A small sensor, is inserted under the skin, typically on the abdomen or arm. The sensor stays in place for up to 2 weeks.
Glucose Measurement: The sensor contains an enzyme called glucose oxidase that reacts with glucose in the interstitial fluid. This reaction produces a small electrical signal that is proportional to the glucose concentration. The sensor measures this signal to estimate glucose levels.
Data Transmission: The sensor wirelessly transmits the glucose data to a receiver or smartphone app. This transmission provides real-time updates on glucose levels throughout the day.
Continuous Monitoring: The CGM system continuously monitors glucose levels, allowing individuals to see how their levels fluctuate in response to meals, exercise, stress, and other factors. Users can view trends, such as rising or falling glucose levels, and take corrective actions if necessary.
Alerts and Alarms: Many CGMs are programmed to send alerts if glucose levels go too high (hyperglycemia) or too low (hypoglycemia), which can help prevent dangerous situations. These alerts can prompt timely intervention to adjust insulin, food intake, or activity.
Data Logging and Analysis: Over time, CGM devices track and store glucose data, which can be reviewed by both the user and their healthcare provider. This information helps to analyze glucose patterns, identify trends, and make informed decisions about lifestyle changes or adjustments to treatment plans.
More recently, CGMs are becoming recognized as a general tool for improving metabolic health. People can track their progress and notice immediate effects of their lifestyle changes— regardless of whether they have diabetes, obesity or want to work on their metabolic health.
Why is a CGM better than other methods of monitoring blood sugar?

A CGM gives you constant accountability. It’s like a coach on your upper arm, reminding you to think before you eat. Many individuals report better dietary compliance simply because they don’t want the negative feedback of a visible glucose rise.
Behavioral change can be difficult. The added accountability that comes with wearing a CGM may be what you need to succeed long term.
Fasting blood sugar is the most commonly used blood sugar measurement in typical medical practices.
Fasting blood sugar (FBS) is the measurement of your blood glucose (sugar) level after you have not eaten or consumed any caloric beverages for at least 8 to 12 hours. This test is commonly used to assess how well your body is managing glucose and is often used to diagnose conditions like diabetes or prediabetes. During fasting, your body relies on stored energy sources, and blood sugar levels should remain relatively stable, as insulin helps regulate glucose. The fasting blood sugar test gives insight into how efficiently your body is processing glucose in the absence of food. Unfortunately, it is likely also the least helpful for early detection of metabolic disease.
Tracking blood sugar variations throughout the day with a CGM provides the opportunity to detect problems earlier.
Is a CGM right for you?

A CGM can be beneficial for several groups of people, especially those with conditions that affect glucose regulation.
Who should consider using a CGM:
People with Type 1 or 2 Diabetes: Individuals with diabetes need to keep their blood sugar in normal range. A CGM makes it easier to improve insulin sensitivity and doses, resulting in a better overal glucose control..
Pregnant women with gestational Diabetes: Women with gestational diabetes can benefit from a CGM as it helps them keep track of their blood glucose levels, allowing for more accurate management to prevent complications during pregnancy for both mother and baby.
Prediabetes: people at risk of developing Type 2 Diabetes: Individuals who are prediabetic or at high risk for type 2 diabetes can use a CGM to track how their body responds to different foods, exercise, and stress. This data can help them make lifestyle changes that could prevent the onset of diabetes.
Obese Individuals: Obesity is a significant risk factor for developing type 2 diabetes. CGMs can help people with obesity monitor their glucose levels, gain insights into how food and exercise affect their metabolism, and guide healthier eating and activity choices.
Athletes and Active Individuals: Athletes or those with intense training routines can use a CGM to track how their workouts affect glucose levels, ensuring they maintain optimal energy and avoid blood sugar imbalances that can hinder performance.
In general, CGMs are suitable for anyone who needs better insights into their glucose levels and wants more control over their metabolic health.
Who should not consider a CGM:
- You are uninterested or unwilling to change your lifestyle.
- You are cost-sensitive and content checking blood sugar once or twice daily.
- You are pregnant, critically ill, or on dialysis. Most company websites state their devices have not been tested and are not appropriate for use with these groups.
- You have a high likelihood of becoming obsessive about the blood sugar reading and engaging in unhealthy dietary practices to achieve a particular glucose level.
Who should use caution with a CGM?
People with Severe Skin Sensitivities or Allergies: The sensor on a CGM is attached to the skin using an adhesive. Individuals who have sensitive skin or are prone to skin reactions, such as rashes or allergic reactions, may experience discomfort or irritation from the adhesive. Those with conditions like eczema, psoriasis, or other chronic skin disorders may have difficulty using a CGM, as these conditions can interfere with the sensor’s adhesion or accuracy. It’s important to discuss options with a doctor if skin issues are present.
Patients using certain medication that affect blood flow (vasoconstrictors), impact glucose regulation or cause dehydration (diuretics) may affect the interstitial fluid and impact the accuracy of CGM readings. Users should work with their healthcare provider to adjust treatment.
Individuals with Poor Blood Flow or Circulation: People with peripheral artery disease (PAD) or other circulation issues may experience problems with CGM sensors, as proper glucose measurements rely on interstitial fluid, which may not be accurately reflected in individuals with compromised circulation.
Pregnant Women Without Medical Supervision: While CGMs can be helpful for pregnant women with gestational diabetes, those who are pregnant and don’t have gestational diabetes, or those without clear medical supervision, should use caution. Any changes in glucose levels during pregnancy should be closely monitored by a healthcare provider to ensure the health of both the mother and the baby.
How to use a CGM to monitor blood sugar
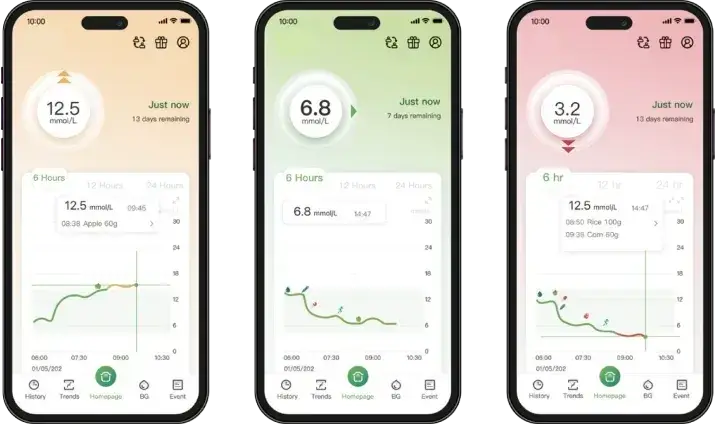
There are multiple ways to use a CGM if you want to learn more about your metabolic health and your body’s response to lifestyle choices. Here are a few ways to use the device.
Make every meal a chance to learn your carb tolerance
Study how your glucose level responds to the food you eat?
- Check your blood sugar before you eat. This is your baseline level.
- Eat a regular meal, or you can design specific meals to test.
- Record your blood sugar values at different time points after eating.
- Ideally, you want your peak post-meal blood sugar to be less than 140 mg/dL (7.8 mmol/L) in diabetes and below 120 mg/dL (6.7 mmol/L) in non-diabetes.
If your blood sugar responds as described, congratulations! You respond well to your chosen meal and can eat it as part of a metabolically healthy diet.
If your blood sugar is higher than desired or consistently takes longer than 2 hours to return to baseline, then try switching up your meal and test again. Consider reducing the number of carbohydrates or add fat and protein to blunt the carbs’ effect.
Make every day a chance to improve your average glucose levels
CGMs calculate your average glucose levels every day, which is more immediate than what a HbA1c test represents (a three month average of blood sugars). Numerous studies show higher HbA1c levels correlate with an increased risk of poor health outcomes. However, interpretation of a HbA1c test result is based on the assumption that red blood cells live 120 days — but this is actually just a rough estimate. Red blood cell lifespan may vary from person to person, which can affect the HbA1c result, making CGM a useful complementary tool.
Make each day a sleep and stress test
Food isn’t the only variable that affects your blood sugar. Poor sleep and poorly managed stress can increase blood sugar levels, regardless of how well you eat.
Exercise and intermittent fasting, on the other hand, can improve your blood sugar levels.
For those individuals, who may experience a stressful workweek, mindfulness practice may have a more significant blood sugar impact than different food choices.
It may be difficult to pinpoint one specific variable since you can’t always control your sleep, your stress, and all your meals. But the more detailed notes you keep, the more information you have to act upon.
Downsides of CGMs
Accuracy
CGMs measure glucose in the tissue fluid just under your skin and these glucose levels can lag behind blood glucose levels by several minutes. Therefore, during a rapid drop or rise in blood sugar, the reading on your CGM may overestimate or underestimate your true blood sugar level, respectively. This can be dangerous if making an insulin dosing decision based off the CGM reading.
Newer CGM models have better accuracy than previous models but still have around a 10% to 20% error margin depending on which manufacturer’s CGM you use.
As technology continues to progress, we expect the accuracy to improve in step.
Price
Most health insurance policies only cover CGMs if you are diabetic on insulin. Prediabetic, obese and active individuals up to date receive no reimbursement from the health insurance companies and have to pay between $70 and $800 for one month of monitoring.
For those concerned about cost, a cheaper blood glucose meter and pricking your finger before each meal and two-to-three times after each meal to get similar information remains an option.
Obsession
CGMs could trigger an obsessive personality trait in which the user focuses on getting a ”flatline” tracing, meaning no rise in blood sugar.
Missing other factors
CGMs could motivate you to eat in a manner that worsens other health parameters for the sake of your blood sugar. Keep in mind that blood sugar is one of many health markers to consider.
Why is it important to monitor blood sugar?

Checking your blood sugar can keep you on your nutrition plan. Most people don’t want to see a high blood sugar number flashing on their screen, reminding them they ate something that makes their blood glucose go up.
Additionally, the data consistently show that elevated blood sugars are associated with a higher risk of heart disease, heart failure, and other harmful diseases — even without a diagnosis of diabetes.
Such variability makes general dietary recommendations less useful for each individual. Instead, a CGM can help you understand what foods help or harm your blood sugar response the most.
Also, CGMs may be the best tools for detecting glucose variability. Higher glucose variability correlates with worse health outcomes and is, therefore, an important measurement to follow.
Next steps: a 4-week plan

First, discuss with your healthcare provider if a CGM is right for you.
Week 1: Once you have your CGM, use the first week as a “monitoring” week. Try not to change your lifestyle in any meaningful way. Record and monitor your blood sugar patterns, merely taking notes without reacting to them.
Weeks 2 and 3: During the next two weeks, experiment with different foods to note how they affect your glucose responses.
You can also experiment with combinations of foods. Once you get a feel for how different foods affect your blood sugar, you can also experiment with exercising before or after eating, going to bed earlier or later, or different lengths of intermittent fasting.
Just remember to change only one thing at a time; otherwise, you will have to guess which action led to the result.
Week 4: During the fourth and final week, implement a new way of eating based on the experiments and compare your results to week one. Hopefully, you have learned which meals you react best to, and you can create a week-long meal plan to try your new way of eating.
Of course, your experiment doesn’t have to end at four weeks. You can choose to continue to wear a CGM long term and continue occasional experiments.
Summary
A continuous glucose monitor is a more comprehensive blood sugar measuring tool than a traditional glucometer. It provides real-time, actionable feedback that you can use to improve your metabolic health.
If you want the most detailed analysis of your blood sugar and to learn as much as you can about how different foods impact your metabolic health, a CGM may be the right choice for you.
Do you want to learn more about CGMs? Please contact us at support@medicfit.nl


